As a middle-aged massage therapist who has spent years helping others find relief from pain, I never expected to find myself grappling with persistent knee discomfort. The irony wasn’t lost on me as I struggled to perform my daily tasks, both at work and at home. My profession, which I love dearly, was becoming increasingly challenging due to the constant ache in my knees. That’s when I stumbled upon RejuvaKnee, and I can confidently say it has been a game-changer for me.
From the moment I first used RejuvaKnee, I felt a sense of hope that had been missing for months. The soothing warmth, gentle massage, and dynamic compression worked in harmony to provide almost immediate relief. As someone who understands the intricacies of bodywork, I was impressed by the device’s thoughtful design and its ability to target multiple aspects of knee pain simultaneously.
Within just a few weeks of consistent use, I noticed a significant improvement in my mobility and a dramatic reduction in pain. I could once again perform my massage techniques with ease and comfort, and my quality of life improved both professionally and personally. The transformation has been so profound that I now find myself recommending RejuvaKnee to many of my clients who struggle with similar issues.
In this review, I’ll share my personal experience with RejuvaKnee, delve into how it works, and explain why I believe it could be a valuable tool for anyone dealing with knee pain. If you’re struggling like I was, I wholeheartedly recommend giving RejuvaKnee a try. It’s been nothing short of transformative for me, and it might just be the solution you’ve been searching for.
What is RejuvaKnee?
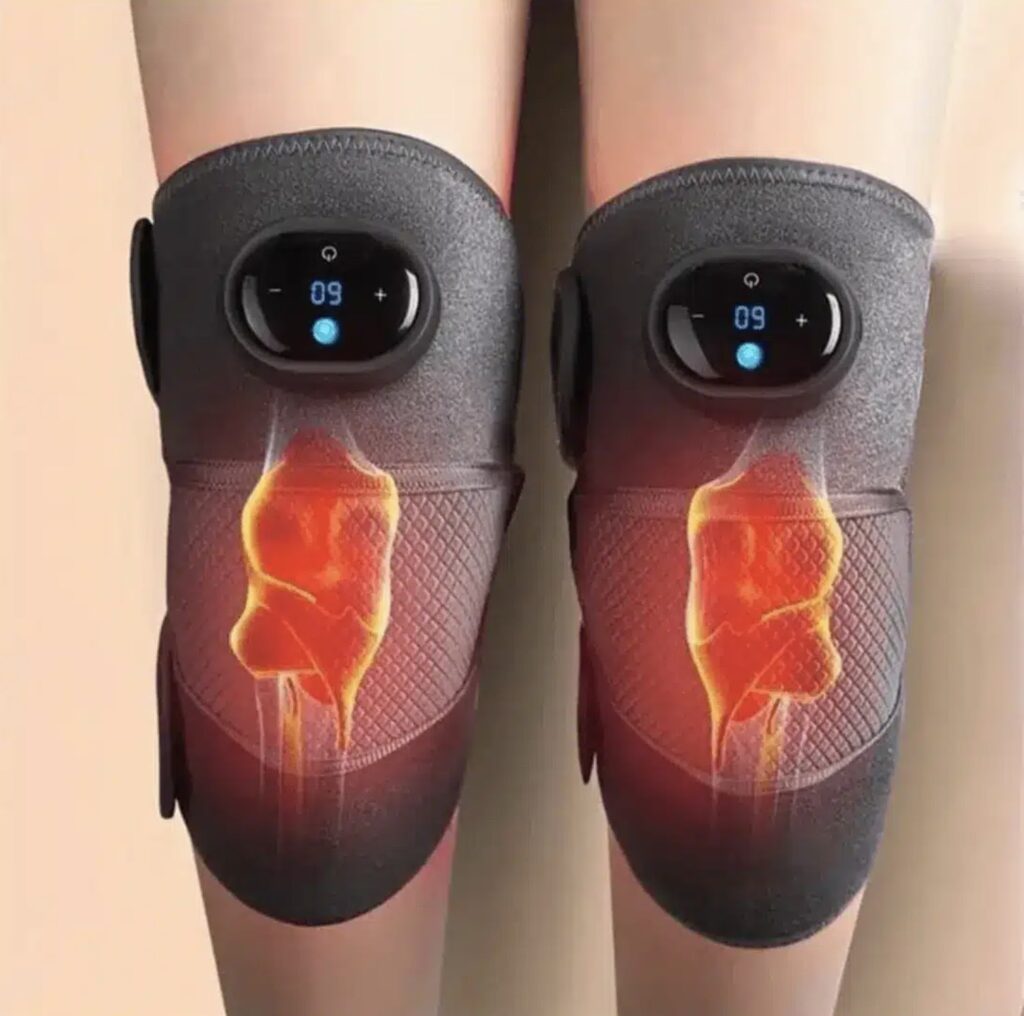
RejuvaKnee is an innovative knee relief device designed to alleviate chronic knee pain, reduce swelling, and increase mobility. This advanced therapeutic device combines three key treatment methods – heat therapy, therapeutic massage, and dynamic compression – to provide effective and long-lasting relief from knee discomfort. Developed by leading knee pain experts, RejuvaKnee offers a non-invasive alternative to painkillers, cortisone shots, and surgery for individuals suffering from various knee issues, including arthritis, injuries, and post-surgery recovery.
How Does It Work
RejuvaKnee employs a “Triple Method” healing approach to target knee pain effectively:
Heat Therapy: The device delivers soothing heat to the knee joint, increasing blood flow and oxygen supply. This enhanced circulation brings essential nutrients to the area, promoting collagen production crucial for cartilage repair.
Therapeutic Massage: RejuvaKnee provides targeted massage to relax tight muscles and tissues around the knee. This helps increase range of motion, reduce pain, and improve overall mobility.
Dynamic Compression: The device applies gentle compression to the knee, which helps control swelling by removing excess fluid and reducing inflammation. This compression also provides additional support to the weakened joint.
The combination of these therapies works synergistically to address the root causes of knee pain rather than merely masking symptoms. Clinical trials have shown impressive results, with 92% of users reporting a significant reduction in pain within the first 15 minutes of use, and 88% experiencing a notable increase in mobility after just 3 days of consistent use.
How to Use RejuvaKnee
Using RejuvaKnee is straightforward and convenient:
- Placement: Fasten the RejuvaKnee device directly on your skin around the affected knee. Ensure it’s snug but not too tight.
- Power On: Press and hold the power button for 3 seconds to activate the device.
- Adjust Settings: Use the touch screen to set your desired heat level and massage intensity. The device offers multiple heat settings ranging from 40°C to 60°C (104°F to 140°F) and three massage speeds.
- Treatment Duration: For optimal results, use RejuvaKnee for at least 15 minutes daily. Many users prefer two 15-minute sessions per day.
Remember to charge the device fully before first use, which takes about 2-3 hours. A full charge provides 1-2 hours of usage time.
RejuvaKnee is designed to be user-friendly and portable, allowing you to use it wherever you need relief. The device comes with additional extension straps to fit even the largest and most swollen legs, making it a one-size-fits-all solution.
For best results, consistent use is key. Most users notice a reduction in pain and swelling, as well as an increase in mobility, from the first use. Continued use will yield even better results, with many reporting significant improvements in their overall quality of life after regular usage.
What I Like About RejuvaKnee
- Immediate pain relief: I felt a noticeable reduction in knee pain within the first 15 minutes of use.
- Versatile treatment options: The combination of heat therapy, massage, and compression allows me to customize my treatment.
- User-friendly interface: The touch screen is intuitive and easy to navigate, even with my not-so-tech-savvy fingers.
- Portable design: I can easily take it with me to work or when traveling, ensuring I never miss a treatment.
- Long battery life: A single charge lasts for multiple sessions, which is perfect for my busy schedule.
- Adjustable fit: The extension straps accommodate my knee perfectly, even on days when swelling is more pronounced.
- Non-invasive solution: As someone wary of medications and surgery, I appreciate this drug-free alternative.
- Quiet operation: I can use it while watching TV or reading without any distracting noise.
What I Don’t Like About RejuvaKnee
- Initial cost: The upfront price is a bit steep, though I now consider it a worthwhile investment.
- Learning curve: It took me a few tries to find the perfect settings for my specific needs.
- Treatment time: While effective, the recommended 15-minute sessions can feel long on particularly busy days.
- Cleaning maintenance: Regular cleaning is necessary to maintain hygiene, which adds to my daily routine.
- Limited to knee area: As effective as it is for knees, I wish it could be used on other joints as well.
- Dependency concern: I worry about becoming too reliant on the device for pain management.
- Charging time: The 2-3 hour charging period can be inconvenient if I forget to charge it overnight.
- Not suitable for all conditions: It may not be appropriate for certain knee injuries or immediately after surgery.
Is RejuvaKnee Legit?
Yes, it’s legit. As a massage therapist, I’ve seen my fair share of wellness products come and go, many of them promising miraculous results but falling short. This experience has made me naturally skeptical of new devices claiming to offer pain relief. However, RejuvaKnee has genuinely impressed me, and I believe it’s a legitimate solution for several reasons.
Firstly, the science behind RejuvaKnee aligns with what I know about pain management and tissue healing. The combination of heat therapy, massage, and compression is a tried-and-true approach that I’ve used in my own practice for years. RejuvaKnee essentially combines these proven techniques into one convenient device, which makes perfect sense from a therapeutic standpoint.
Secondly, I’ve experienced the results firsthand. The relief I felt wasn’t just a placebo effect – I noticed tangible improvements in my mobility and a significant reduction in pain. As someone who relies on my body for my livelihood, I’m acutely aware of changes in my physical condition, and the positive changes brought about by RejuvaKnee were undeniable.
Moreover, I’ve recommended RejuvaKnee to several of my clients, and their feedback has been overwhelmingly positive. Seeing others benefit from the device in the same way I have further solidifies my belief in its legitimacy. The consistency of positive results across different individuals with varying degrees of knee issues speaks volumes about the product’s effectiveness.
Lastly, the company behind RejuvaKnee appears to be transparent about their product. They provide clear information about how the device works, offer a reasonable return policy, and don’t make exaggerated claims about overnight miracles. This level of honesty is refreshing in an industry often plagued by overpromising and underdelivering.
While I understand that no solution works for everyone, my personal and professional experience with RejuvaKnee has convinced me of its legitimacy as a valuable tool for managing knee pain and improving mobility.
Where to Buy RejuvaKnee
After experiencing such incredible results with RejuvaKnee, I’m often asked where to purchase it. My advice is always the same: buy directly from the RejuvaKnee official store. This ensures you’re getting an authentic product backed by their excellent customer service and warranty.
Plus, the official store frequently offers special promotions and discounts that you won’t find elsewhere. Trust me, it’s worth going straight to the source for this life-changing device. Don’t risk buying from unauthorized sellers – stick with the official RejuvaKnee store for peace of mind and the best deal possible.